Home Features The Science of COVID-19: COVID-19 and Mental Health
Contributed by:
Dr. Davendranand Sharma
Professor of Behavioral Health
The World Health Organization (WHO) predicts that the next pandemic would be a crisis in mental health disorders. Mental health includes emotion, cognition (thought process), behavior, and the personality of the individual, which all originate in the brain. 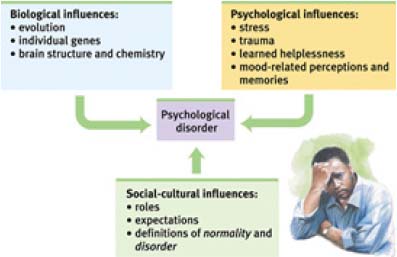
Abnormal reaction to any one of the components of mental health can occur by three main mechanisms: gene influences, the influence of past experiences of trauma and conflict present in the unconscious, and external stressors.
External stressors are often by events out of the control of the individual, which can impact the brain leading to emotional, cognitive and behavioral disorders.
The COVID-19 crisis is an event which came unexpectedly and has led to significant changes to the lives of everyone, including children, who have to adjust to a new way of life that disrupts their social development in school and play.
The COVID-19 crisis can affect an individual’s brain, causing mental health disorders in a number of ways: directly by the viral impact on the affected persons’ immune system and also by changes in brain function by direct entry into the brain, causing a wide variety of neurological problems, including delirium and vascular disorders.
Neurochemical changes occur which can lead to emotional problems and behavior problems, including aggressive behavior and confusion. Impulse control disorders and addiction disorders are included in the behavioral disorders; anxiety and depression in the emotional disorders; and poor concentration, overthinking and worrying in the cognitive disorders.
Indirect effects are the secondary consequences of the COVID-19 crisis. Depression and anxiety are felt as a reaction to financial difficulties and social isolation. Changes in schedules may cause sleep disorders with increasing tiredness during the day.
A marked decrease in recreational activities may lead to family tension and persons may experience increased irritability and mood changes. Compensatory overuse of cell phones, which some persons are on for many hours of the day, can cause brain wave changes and in some cases seizure episodes.
Fear of contracting the COVID-19 virus and dying can lead to panic attacks where persons experience short bursts of heart racing, shortness of breath, increased sweating, feeling as if everything is unreal, and experiencing extreme fear.
Persons of different age groups show different reactions. The elderly, who are a vulnerable group, experience depression, which is insidious and presents quiet worry, loss of appetite, fatigue, and sometimes hopelessness with thoughts of dying.
Working adults generally would experience more anxiety related to finances and parenting, with concerns about contracting the viral illness, leading to obsessional extreme cleansing and phobias, including fear of contamination.
Children
Children of different age groups show different responses. Young children age 1 to 6 years can experience helplessness, fear, sleep terror, nail biting and depression, manifested by withdrawal from social activities. Older children and adolescents may show mood changes, more social isolation, loneliness, anxiety and obsessional diversion by cell phone overuse.
The psychological consequences of the COVID-19 crisis can also be divided into acute and chronic effects, and can also be experienced by health workers and by those who are affected indirectly, such as the family of the patients who succumb to the illness.
Acute effects include emotional shock, acute grief reactions and acute stress disorders. These reactions consist of an intense period of confusion, disbelief, denial, anxiety, agitation and mood changes.
Feelings of de-realization and depersonalization may also occur and people often talk about this experience as being unreal and feel that it is a bad dream from which they would wake up and find life as before. The time frame for acute reactions depends on the individual’s personality, life experiences, maturity, coping capacity, and professional support received.
Generally, acute reactions continue to be intense for several days and would usually last up to a month, during which time the individual would go through the stages of grief, denial, anger, bargaining, depression, and hopefully come to accept the reality of the horrific pandemic and associated loss which allows for resolution of symptoms. Supportive counseling is the usual method of helping individuals through this period.
However, if a grief reaction continues to be intense after the first month and is associated with abnormal symptoms, including hallucinations, alcohol abuse, prolonged depression or persistence of denial and anger, this would be pathological grief and would require specialist treatment.
PTSD
Health workers are prone to experiencing “burn out” when their cognitive capacity could be compromised resulting in problems with judgment. Acute stress reactions which persist for more than a month are called post traumatic stress disorder (PTSD), which is a serious consequence.
Post traumatic stress disorder, if untreated, causes significant distress and is associated with substance abuse disorders, especially alcohol abuse and dependence. Common symptoms of this disorder include feelings of de-realization and de-personalization, depressed mood, persistent high anxiety or arousal states, and nightmares.
Avoidance behaviors could include fear of going outdoors and obsessive cleansing. Individuals who are particularly prone to developing this disorder include children, the elderly, people with mental health problems, and frontline workers themselves.
Frontline workers are a special group of vulnerable people primarily because of the denial of their own emotional feelings and the use of defenses like isolation of emotions to cope with the enormity of the crisis and to try to remove unpleasant visual images and memory.
Unfortunately, these defenses result in emotional numbing. PTSD and may lead to alcohol abuse in an effort to block out painful memories. The management of PTSD requires specialist treatment and involves primarily psychotherapy, including treatment of associated conditions like substance abuse.
Psychological consequences can be mitigated in their intensity by adequate preparation and response. This should include public education on stress management and information on the availability of support systems and on how to access these services.
The training of personnel to be able to recognize and deal effectively with emotional reactions is of value. Utilizing psychological first aid for frontline workers involved in the crisis may help to prevent stress reactions in persons providing relief and care.
A national Mental Health and Psychosocial Support system (MHPSS) is recommended by the WHO and PAHO as valuable for preventing and managing emotional and other mental health problems associated with the COVID-19 crisis.
Article submitted as part of the Ministry of Health’s COVID-19 public information and education programme
